As we age, we gain wisdom, but we also face an increased risk of serious health issues, such as cancer, heart disease, and Alzheimer’s. Among these health concerns lurks another silent epidemic: kidney disease, particularly for those with high blood pressure or diabetes, which poses an even greater threat to African American and Native American populations.
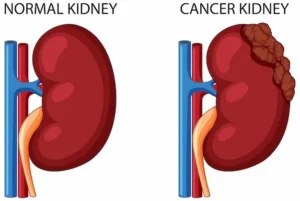 Startlingly, over 20 million Americans remain oblivious to their moderate chronic kidney disease, as reported by the National Kidney Foundation, with an additional 20 million at risk. However, there is a glimmer of hope in these daunting statistics. Dr. Walter F. Piering, a specialist in nephrology and a Professor of Medicine at the Medical College of Wisconsin, emphasizes that “most kidney disease can be prevented.”
Startlingly, over 20 million Americans remain oblivious to their moderate chronic kidney disease, as reported by the National Kidney Foundation, with an additional 20 million at risk. However, there is a glimmer of hope in these daunting statistics. Dr. Walter F. Piering, a specialist in nephrology and a Professor of Medicine at the Medical College of Wisconsin, emphasizes that “most kidney disease can be prevented.”
This critical insight highlights the need for early detection and intervention, as untreated cases may eventually lead to kidney failure. The primary culprits behind kidney disease are diabetes and high blood pressure, accounting for approximately two-thirds of all new cases.
Connective tissue disorders like lupus erythematosus, untreated urinary tract infections, and streptococcal infections, particularly in children, can also impair kidney function, although these causes are relatively uncommon. Kidney cancer, or nephroma, represents less than 2% of all adult cancers, while kidney failure due to injury or poisoning remains rare.
Optimizing Kidney Health: Kidney Function Tests (KFT)

The kidneys, essential organs responsible for eliminating metabolic wastes and maintaining water and electrolyte balance, play a critical role in our overall well-being. To gauge the efficiency of your kidneys, kidney function tests (KFT) are conducted, assessing how effectively your kidneys remove waste from your body. These tests may involve a 24-hour urine sample, a blood test, or both.
Importance of Kidneys:
Positioned just below your left rib cage at the back of your abdomen, your kidneys serve several vital functions. Besides waste elimination, they produce hormones that regulate blood pressure, create red blood cells for oxygen transport, and generate vitamin D for bone and muscle health. Keeping your kidneys healthy is of utmost significance, and undergoing regular kidney function tests is a reliable way to monitor your well-being.
Symptoms of kidney problems:
 Various symptoms may indicate kidney issues, such as frequent urination, difficulty initiating urination, painful urination, high blood pressure, blood in the urine, and swelling of the hands and feet. However, it’s essential to remember that a single symptom may not always signal a severe problem.
Various symptoms may indicate kidney issues, such as frequent urination, difficulty initiating urination, painful urination, high blood pressure, blood in the urine, and swelling of the hands and feet. However, it’s essential to remember that a single symptom may not always signal a severe problem.
Different Types of Kidney Function Tests (KFT):
To assess kidney health accurately, physicians may prescribe different kidney function tests. Some common tests include:
- Serum creatinine: This waste product of metabolism is eliminated by the kidneys. Elevated creatinine levels may indicate kidney problems.
- Uric Acid: The breakdown of organic compounds generates uric acid, which the kidneys filter and excrete. Abnormal levels may signal kidney damage.
- Blood Urea Nitrogen (BUN): Produced when the body breaks down proteins, urea nitrogen is eliminated by the kidneys. Elevated BUN levels could be linked to kidney issues or certain medications.
- Electrolytes: These minerals in the blood and body fluids play a crucial role in various bodily functions and are indicators of kidney function.
- Estimated Glomerular Filtration Rate (eGFR): This test calculates the kidneys’ ability to filter waste and provides insight into kidney damage.
Additional tests, like microalbuminuria and urinalysis, can help identify specific kidney issues.
Purpose of Kidney Function Tests:
Kidney function tests are essential for individuals with conditions like diabetes, high blood pressure, or symptoms suggestive of kidney problems. Regular testing is especially crucial for those with a family history of kidney-related issues, older individuals, or heavy smokers.
Performing kidney function tests:
The tests usually involve a 24-hour urine sample and blood tests. The urine sample determines creatinine clearance, while blood tests assess various indicators of kidney function.
Understanding Kidney Function and Failure
Healthy kidney function is vital for maintaining overall health. Each day, our bodies extract nutrients from the food we consume for energy and self-repair. After this process, waste materials, including those generated from the breakdown of active tissues, enter the blood.
The kidneys, located near the middle of the back, just below the rib cage, act as sophisticated filtering and reprocessing machines. Processing about 200 quarts of blood daily, these bean-shaped organs sift out approximately two quarts of waste products and excess water, which become urine.
The urine is then stored in the bladder until it is expelled through urination. Failure to eliminate these wastes leads to their buildup in the blood, causing damage.
Simple and Inexpensive Detection
Detecting impaired kidney function is both simple and inexpensive. Dr. Piering stresses the importance of two straightforward tests: a blood pressure check and a urinalysis. He urges patients to insist on these tests during every doctor’s visit, as they can be easily performed by a nurse or medical assistant. Additionally, many health fairs offer these tests, making them more accessible.
The urinalysis involves collecting a small sample of urine in a cup, which is then quickly tested for protein—an indicator of kidney disease. This straightforward test can make a significant difference in identifying potential kidney problems.
Confronting Diabetes and Hypertension
Diabetes remains the leading cause of chronic kidney failure in the United States, responsible for 33% to 40% of new cases each year. Persistently high blood sugar damages the kidneys’ filtering mechanisms, hindering waste and fluid removal.
Similarly, uncontrolled or poorly managed high blood pressure ranks as the second-leading cause of chronic kidney failure in the country, contributing to 27% to 30% of all cases. Elevated blood pressure strains the heart and damages blood vessels, including those in the kidneys, creating a harmful cycle of escalating health issues.
Prevention: A Path to Kidney Health

The encouraging news is that most kidney diseases can be prevented with proper care. Managing conditions like hypertension and diabetes is crucial, and new guidelines recommend stricter blood pressure levels than the traditional 140/90. Maintaining readings at 135/85 or lower for individuals diagnosed with high blood pressure is advised.
Similarly, diabetics should aim for a blood pressure reading of 130/80 or lower. Additionally, those diagnosed with reduced kidney function should strive to keep their blood pressure at 125/75 or lower, according to the National Heart, Lung, and Blood Institute.
Addressing Obesity and Childhood Health
Obesity is a known risk factor for various health conditions, including hypertension and diabetes. With an increasing number of children facing obesity, regular blood pressure and urine checks are vital to assess their risk of hypertension, diabetes, and kidney dysfunction. Early detection and intervention in childhood can pave the way for healthier lives.
Take Charge of Your Kidney Health

Regular blood pressure and urine checks can be fundamental steps towards safeguarding your kidney health. If you are at risk for kidney disease, diabetes, or hypertension, work closely with your healthcare provider to develop a tailored program of diet and medication to prevent potential health threats. Empowering yourself with knowledge and taking proactive measures can make a significant difference in preventing kidney disease.
Let’s come together to raise awareness about kidney disease and take action to promote kidney health. This article draws insights from the National Kidney Foundation, the National Institutes of Health (National Institute of Diabetes and Digestive and Kidney Diseases), and the National Heart, Lung, and Blood Institute. It serves as a call to action to prevent and combat kidney disease in our communities.
Stages of Kidney Disease:
Chronic kidney disease (CKD) evolves through multiple stages, each with its own set of signs and symptoms. The eGFR (estimated glomerular filtration rate) test determines how well your kidneys remove waste and surplus fluid from your blood. It is critical to understand these stages to manage and preserve kidney function. Let’s go over each stage in detail to get a better understanding:
Stage 1 of Chronic Kidney Disease (CKD):
In Stage 1, your kidneys exhibit a normal eGFR of 90 or greater, and you may experience mild kidney damage. At this early stage, your kidneys still function well, and you might not display any noticeable symptoms. However, there could be signs of kidney damage, such as the presence of protein in your urine. It is crucial to take proactive measures to protect your kidney health and prevent further deterioration.
Stage 2 of Chronic Kidney Disease (CKD):
Stage 2 is characterized by a mild decrease in kidney function, with an eGFR between 60 and 89. While kidney damage may progress slightly, your kidneys are still functioning reasonably well. Similar to Stage 1, you might not experience noticeable symptoms, but monitoring your kidney health becomes increasingly important.
Stage 3 of Chronic Kidney Disease (CKD):
In Stage 3, the eGFR ranges from 30 to 59, indicating moderate damage to your kidneys. At this point, your kidneys struggle to effectively filter waste and extra fluid from your blood, leading to potential health problems like high blood pressure and bone disease. Symptoms may start to manifest, such as fatigue, weakness, and swelling in the hands or feet. Stage 3 CKD is further divided into two substages based on eGFR:
- Stage 3a: eGFR between 45 and 59
- Stage 3b: eGFR between 30 and 44
Despite the progression, with appropriate medical care and lifestyle changes, many individuals can prevent further deterioration and avoid reaching Stage 4 or Stage 5.
Stage 4 of Chronic Kidney Disease (CKD):
Stage 4 is a critical phase, indicating severe kidney damage, with an eGFR ranging from 15 to 29. Your kidneys’ ability to filter waste and fluids is significantly impaired, leading to the accumulation of toxins in your body. At this stage, you may experience more pronounced symptoms and require medical interventions to manage the condition effectively.
Stage 5 of CKD (End-Stage Renal Disease, ESRD):
Stage 5 represents the most advanced and critical stage of CKD, with an eGFR of less than 15. At this point, your kidneys have lost almost all functionality, necessitating immediate medical attention. End-stage renal Disease (ESRD) requires life-sustaining treatments such as dialysis or kidney transplantation to replace kidney function.
Determining Your Chronic Kidney Disease Stage:
Doctors use various tests, including eGFR tests and urine analysis, to accurately determine your CKD stage. The eGFR test estimates kidney function, while urine tests provide insights into kidney health. However, it’s essential to note that the current eGFR calculation includes factors like age, sex, and race, among others. A task force led by the National Kidney Foundation (NKF) and the American Society of Nephrology (ASN) is actively working to refine the eGFR calculation and remove race as a factor, ensuring more accurate and unbiased testing.
Fighting Against Kidney Disease:
Organizations like the American Kidney Fund (AKF) are dedicated to supporting individuals living with kidney disease and those at risk. From prevention to post-transplant living, AKF strives to provide assistance, advocate for equitable healthcare, and improve the quality of life for millions of Americans affected by kidney disease.
Everyone needs to be aware of the stages of kidney disease and the significance of early detection and intervention. By understanding and taking proactive steps to protect kidney health, we can collectively combat kidney disease and promote better overall well-being.
Chronic Kidney Diseases: Causes and Complications
Chronic kidney disease (CKD) is a serious health condition that requires careful management and early detection. Dr Andrew Bentall, a kidney specialist at Mayo Clinic, sheds light on CKD, its causes, symptoms, diagnosis, and treatment options in this informative video. Whether you’re seeking answers for yourself or a loved one, this guide aims to provide you with the most accurate and up-to-date information.
Chronic kidney diseases can be a serious health concern, but there’s good news: you can take steps to prevent them. Let’s delve into the factors that cause these conditions and explore the potential complications they can lead to.
What is chronic kidney disease?
CKD is characterized by progressive damage and loss of function in the kidneys. Surprisingly, about one in seven American adults is affected by this condition, with many unaware of their diagnosis.
To grasp the implications of CKD, let’s first understand the essential roles our kidneys play in maintaining bodily balance. These vital organs remove waste, toxins, and excess water from our blood, which is then eliminated through urine. Additionally, kidneys produce hormones, and red blood cells, and activate vitamin D for body usage.
Causes and Risk Factors of CKD:
CKD can result from various factors, some unavoidable, while others are within our control. Genetic conditions like polycystic kidney disease and autoimmune disorders such as lupus or IgA nephropathy increase the risk.
Age, kidney structure defects, and family history are also contributing factors. Common medical conditions like diabetes, heart disease, and obesity can exacerbate kidney damage. Additionally, heavy or prolonged use of certain medications and smoking can further raise the risk.
What triggers chronic kidney diseases?
The root cause of chronic kidney diseases lies in the impairment of kidney function. Several factors can contribute to this condition, including:
- Type 1 or Type 2 diabetes: If you have diabetes, your risk of developing kidney problems increases significantly.
- High blood pressure: Uncontrolled high blood pressure can put a strain on your kidneys, leading to long-term damage.
- Recurrent Kidney Infections (Pyelonephritis): Frequent kidney infections can gradually harm the kidneys and affect their ability to function properly.
- Polycystic Kidney Disease: A genetic condition where fluid-filled cysts form in the kidneys, leading to impairment over time.
- Urinary Tract Obstructions: Conditions like an enlarged prostate, kidney stones, or certain cancers can block the flow of urine, causing damage to the kidneys.
- Vesicoureteral Reflux: This condition causes urine to flow back into the kidneys, potentially causing damage and infection.
- Glomerulonephritis: Inflammation of the kidney’s filtering units can affect their ability to remove waste from the blood.
- Interstitial Nephritis: Inflammation of the kidney’s tubules and surrounding structures can hamper their normal function.
Potential Complications of Chronic Kidney Disease:
Chronic kidney diseases can have far-reaching effects on your overall health, leading to various complications.
- Cardiovascular Disease: Kidney problems can increase the risk of heart and blood vessel issues.
- Weak Bones and Fractures: Your bones may become more vulnerable to fractures due to kidney disease-related mineral and hormone imbalances.
- Anaemia: Decreased production of red blood cells can lead to anemia, causing fatigue and weakness.
- Sexual and Reproductive Issues: Kidney problems might reduce sex drive, lead to erectile dysfunction, or impact fertility.
- Central Nervous System Damage: Difficulty concentrating, personality changes, and even seizures can occur due to kidney-related central nervous system issues.
- Weakened Immune System: Impaired kidneys can lower your body’s ability to fend off infections.
- Pericarditis: Inflammation of the membrane around the heart can cause chest pain and discomfort.
- Pregnancy Complications: For expectant mothers with kidney diseases, there can be risks for both the mother and the developing fetus.
- End-Stage Kidney Disease: In severe cases, kidney damage becomes irreversible, necessitating dialysis or a kidney transplant for survival.
- Fluid Retention: Kidney problems may lead to swelling in your arms and legs, high blood pressure, or fluid in your lungs.
- Hyperkalemia: A sudden rise in potassium levels can impair heart function and pose life-threatening risks.
In some unfortunate cases, chronic kidney diseases can even lead to death. understanding the causes and potential complications of chronic kidney diseases is crucial for prevention and early intervention. By managing risk factors and making healthy lifestyle choices, you can protect your kidneys and promote overall well-being.
Symptoms and Diagnosis Chronic Kidney Disease (CKD):
Early stages of CKD may show no visible symptoms, making early detection difficult. However, if the disease advances, nausea, vomiting, muscular cramps, loss of appetite, swelling in the feet and ankles, dry, itchy skin, shortness of breath, and changes in urine patterns may occur. Regular medical visits are essential because normal blood tests can detect early signs of CKD. Interventions can be implemented to slow the progression if found early.
A series of tests, including eGFR and urine analysis, are commonly used to make a diagnosis. Ultrasounds or CT scans, for example, may be used to evaluate kidney size, structure, and visual damage. In some circumstances, a kidney biopsy may be required for additional investigation.
Treatment Options for Chronic Kidney Disease (CKD):
Treating the cause of CKD is crucial to reducing complications and slowing disease progression. For instance, better control of blood pressure, improved sugar management in diabetes, and weight reduction are vital interventions.
Although existing kidney damage may not be reversible, treatment can help manage the condition and improve the quality of life. Medications to control blood pressure, reduce fluid retention, alleviate anaemia, lower cholesterol, and protect bones and blood vessels may be prescribed. In some cases, a low-protein diet may be recommended.
End-Stage Kidney Failure and Beyond:
When CKD has advanced to end-stage kidney failure, where 85 to 90 percent of kidney function is lost, dialysis or a kidney transplant becomes necessary for survival. Dialysis involves filtering toxins and removing excess water from the body through a machine. A kidney transplant, if eligible, is often the preferred option, as it offers the closest chance to a cure.
Lifestyle Choices and Coping:
If you have CKD, lifestyle choices play a crucial role in managing the condition. Quitting smoking, moderating alcohol consumption, maintaining a healthy weight, and staying active can positively impact kidney health. Emotional support is essential, and talking to a trusted friend, relative, or therapist, or joining a support group can be beneficial.
Can Kidney Function Improve?
Early diagnosis of kidney disease allows for appropriate treatment, and certain interventions can delay or prevent kidney failure in severe cases. Maintaining blood pressure, blood glucose, and cholesterol within target ranges, following a balanced diet, staying physically active, taking prescribed medications, and getting regular kidney function tests all contribute to kidney health.
Are Kidney Function Tests Risky?
Kidney function blood tests are generally safe, with no significant risks. Some individuals may experience mild discomfort during blood collection.
Prioritizing kidney health is essential for overall well-being. Regular kidney function tests are valuable tools for detecting potential kidney issues early on. Alongside a healthy lifestyle, proper monitoring can contribute to better kidney health.
Conclusion
In conclusion, understanding CKD and seeking early detection and intervention are vital steps in managing this condition. By implementing necessary lifestyle changes and adhering to medical advice, individuals with CKD can lead more comfortable and fulfilling lives. For more information on CKD, explore our related videos. We wish you well on your journey to kidney health.